EP0182520A2 - Apparatus for iontophoretic drug delivery - Google Patents
Apparatus for iontophoretic drug delivery Download PDFInfo
- Publication number
- EP0182520A2 EP0182520A2 EP85307771A EP85307771A EP0182520A2 EP 0182520 A2 EP0182520 A2 EP 0182520A2 EP 85307771 A EP85307771 A EP 85307771A EP 85307771 A EP85307771 A EP 85307771A EP 0182520 A2 EP0182520 A2 EP 0182520A2
- Authority
- EP
- European Patent Office
- Prior art keywords
- drug
- electrode
- species
- source
- electrode assembly
- Prior art date
- Legal status (The legal status is an assumption and is not a legal conclusion. Google has not performed a legal analysis and makes no representation as to the accuracy of the status listed.)
- Granted
Links
Images
Classifications
-
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61N—ELECTROTHERAPY; MAGNETOTHERAPY; RADIATION THERAPY; ULTRASOUND THERAPY
- A61N1/00—Electrotherapy; Circuits therefor
- A61N1/02—Details
- A61N1/04—Electrodes
- A61N1/0404—Electrodes for external use
- A61N1/0408—Use-related aspects
- A61N1/0428—Specially adapted for iontophoresis, e.g. AC, DC or including drug reservoirs
- A61N1/0432—Anode and cathode
- A61N1/0436—Material of the electrode
-
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61N—ELECTROTHERAPY; MAGNETOTHERAPY; RADIATION THERAPY; ULTRASOUND THERAPY
- A61N1/00—Electrotherapy; Circuits therefor
- A61N1/02—Details
- A61N1/04—Electrodes
- A61N1/0404—Electrodes for external use
- A61N1/0408—Use-related aspects
- A61N1/0428—Specially adapted for iontophoresis, e.g. AC, DC or including drug reservoirs
- A61N1/0448—Drug reservoir
-
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61N—ELECTROTHERAPY; MAGNETOTHERAPY; RADIATION THERAPY; ULTRASOUND THERAPY
- A61N1/00—Electrotherapy; Circuits therefor
- A61N1/02—Details
- A61N1/04—Electrodes
- A61N1/0404—Electrodes for external use
- A61N1/0408—Use-related aspects
- A61N1/0428—Specially adapted for iontophoresis, e.g. AC, DC or including drug reservoirs
- A61N1/0444—Membrane
Landscapes
- Engineering & Computer Science (AREA)
- Health & Medical Sciences (AREA)
- Bioinformatics & Cheminformatics (AREA)
- Life Sciences & Earth Sciences (AREA)
- Nuclear Medicine, Radiotherapy & Molecular Imaging (AREA)
- Radiology & Medical Imaging (AREA)
- Biomedical Technology (AREA)
- Animal Behavior & Ethology (AREA)
- General Health & Medical Sciences (AREA)
- Public Health (AREA)
- Veterinary Medicine (AREA)
- Pharmacology & Pharmacy (AREA)
- Electrotherapy Devices (AREA)
- Medicinal Preparation (AREA)
Abstract
Description
- This invention relates to improvements in iontophoretic drug delivery, particularly to iontophoretic drug delivery apparatus for transdermal medicament delivery and to improvements therein. More specifically, this invention relates to improved apparatus for active (as opposed to passive) transdermal, ambulatory, drug delivery. Yet more particularly, this invention relates to increased efficiency iontophoresis devices or appliances and to improved methods of making and using such devices.
- Iontophoresis, according to Dorland's Illustrated Medical Dictionary, is defined to be "the introduction, by means of electric current, of ions of soluble salts into the tissues of the body for therapeutic purposes." Iontophoretic devices have been known since the early 1900's. GB-A-410,009(1934) describes an iontophoretic device which overcame one of the disadvantages of such early devices known to the art at that time, namely the requirement of a special low tension (low voltage) source of current which meant that the patient needed to be immobilized near such a source. The device of that British specification was made by forming from the electrodes and the material containing the medicament or drug to be delivered transdermally, a galvanic cell which itself produced the current necessary for iontophoretically delivering the medicament. This ambulatory device thus permitted iontophoretic drug delivery with substantially less interference with the patient's daily occupation.
- More recently, a number of United States patents have issued in the iontophoresis technology, indicating a renewed interest in this mode of drug delivery. For example, US-A-3,991,755 issued to Jack A. Vernon et al; US-A-4,141,359 issued to Stephen C. Jacobson et al; US-A-4,390,545 issued to Wilson; US-A-4,250,878 issued to Jacobsen disclose examples of iontophoretic devices and some applications thereof. The iontophoresis process has been found to be useful in the transdermal administration or introduction of medicaments or drugs including lidocaine hydrochloride, hydrocortisone, acetic acid, fluoride, penicillin, dexamethasone sodium phosphate and many other drugs. Perhaps the widest use of iontophoresis is that of diagnosing cystic fibrosis by using pilocarpine nitrate iontophoresis. The pilocarpine nitrate stimulates sweat production; the sweat is collected and analyzed for its chloride content to detect the presence of the disease.
- In presently known iontophoretic devices, at least two electrodes are generally used. Both these electrodes are disposed so as to be in intimate electrical contact with some portion of the skin of the body. One electrode, called the active electrode, is the electrode from which the ionic substance, medicament, drug precursor or drug (hereinafter "the ionic drug species") is delivered or driven into the body by electrical repulsion. The other electrode, called the indifferent or ground electrode, serves to close the electrical circuit through the body. In conjunction with the patient's skin contacted by the electrodes, the circuit is completed by connection of the electrodes to a source of electrical energy, e.g. a battery or appropriately modified household current. For example, if the ionic substance to be driven into the body is positively charged, then the positive electrode (the anoide) will be the active electrode and the negative electrode (the cathode) will serve to complete the circuit. If the ionic substance to be delivered is negatively charged, then the negative electrode will be the active electrode and the positive electrode will be the indifferent electrode.
- Furthermore, existing iontophoresis devices generally require a reservoir or source of the ionized or ionizable species (or a precursor of such species) - ie the ionic drug species - which is to be iontophoretically delivered or introduced into the body. Examples of such reservoirs or sources of ionized or ionizable species include a pouch as described in the previously mentioned Jacobsen US-A-4,250,878, or the pre-formed gel body of US-A-4,383,529 (Webster). Such drug reservoirs, when electrically connected to the anode or the cathode of an iontophoresis device to provide a fixed or renewable source of one or more desired species, are generally used with anodes or cathodes which are substantially electrochemically inert. As is more fully discussed below, utilization of such substantially inert electrodes as contemplated in the prior art generally has significant disadvantages.
- It is an object of the present invention to enhance the efficiency of the iontophoretic delivery of ionized or ionizable medicaments e.g., drugs, by means of the selection and utilization of a combination of anode or cathode conductive members or electrodes having specified characteristics and of the drug(s) to be delivered. Further subsidiary objects of the invention were to increase the safety and acceptability of the iontophoretic drug delivery process.
- According to one aspect therefore the present invention provides an iontophoretic drug delivery apparatus having an electrode assembly comprising an electrode member in electrical connection to a source for an ionic drug species to be delivered iontophoretically and for counterions therefor, characterized in that said electrode assembly contains at least one electrochemically active component in electrical connection to said source and in that said electrode assembly contains at least one electrochemically active component in electrical connection to said source and in that at least one of said electrochemically active component and said counterions is such that in the operation of said apparatus water electrolysis at said electrode member is substantially avoided and/or ionic products of water electrolysis at said electrode member are substantially neutralized.
- In a preferred embodiment of the invention the electrode assembly of the apparatus includes a component which is electrochemically active during iontophoretic drug delivery to produce a first species which, with a second species employed in or generated during the operation of said apparatus, is capable of interacting to produce a product which is not sufficiently influenced by electrical fields to be iontophoretically introduced.
- According to a further aspect of the present invention there is provided an iontophoretic drug delivery electrode assembly comprising an electrode member in electrical connection to a source for an ionic drug species to be delivered iontophoretically and for counterions therefor, characterized in that said assembly contains at least one electrochemically active component in electrical connection to said source and in that at least one of said electrochemically active component and said counterions is such that in the operation of said assembly water electrolysis at said electrode member is substantially avoided and/or ionic products of water electrolysis at said electrode member are substantially neutralized.
- Viewed from another aspect the iontophoretic drug delivery electrode assembly of the invention comprises an electrode member in electrical connection to a source for an ionic drug species to be delivered iontophoretically and for counterions therefor, characterized in that said assembly contains at least one electrochemically active component in electrical connection to said source and in that at least one of said electrochemically active component and said counterions is such that in the operation of said assembly generation of ionic species at said electrode member is substantially avoided or ionic species generated at said electrode member are substantially entirely converted by species present or generated in or at said source and/or said electrochemically active component into species having lower susceptibility to iontophoretic delivery from said assembly.
- Briefly the present invention permits a method of iontophoretic drug delivery wherein the drug to be iontophoretically delivered, an electrochemically active component of the drug delivery apparatus, or both, are selected so that during operation of the device, the production of unwanted ionic species may be minimized.
- In a preferred embodiment of this invention, the drug to be iontophoretically delivered, an electrochemically active component of the apparatus or both may be selected to reduce the formation of unwanted water electrolysis products during operation of the device. In yet another embodiment of this invention, the drug to be delivered, an electrochemically active component of the iontophoresis apparatus or both, may be selected so as to reduce the presence of water electrolysis products after they are formed.
- As contemplated herein, an electrochemically active component of an iontophoresis device is a part of the device which is oxidized or reduced during iontophoretic drug delivery or which oxidizes or reduces other avilable species. Conveniently, the electrochemically active component may be an electrical current distribution member of the apparatus or a component in the source.
- The present invention also contemplates improved bioelectrodes particularly suited for use with an iontophoresis device or appliance. The improved electrode of this invention provides an iontophoretic device which exhibits enhanced coulombic efficiency in drug delivery processes.
- The electrode asembly conveniently comprises a reservoir containing the medicament to be iontophoretically delivered, the reservoir being in electrical connection with an electrochemically active component, e.g. an active current distribution member, the species produced from the electrochemically active component during operation of the device interacting with the medicament of the reservoir during iontophoretic drug delivery so as to minimize the formation and delivery of undesired species, the electrochemically active component being in further electrical connection with a source of electrical energy. In a preferred embodiment, the electrode assembly includes means for securing the assembly to skin so as to permit iontophoretic drug delivery therefrom.
- The apparatus of the present invention enables a method of iontophoretic drug delivery having enhanced coulombic efficiency to be performed, the method comprising: selecting the ionic species (e.g. a drug) to be iontophoreticaly delivered, incorporating the ionic species into an electrode assembly (e.g. in its medicament reservoir); selecting the composition or construction of either the anode or the cathode of the iontophoresis apparatus to include an electrochemically active component so that the electrochemical reaction at the anode or the cathode produces species which interact with the ionic species so as to reduce the formation of undesired ions; placing the selected anode or cathode in electrical connection with the ionic species (e.g. in connection with the reservoir) and with a source of electrical energy; and transdermally delivering the selected ionic species into the body while minimizing the formation and transdermal delivery of undesired ions.
- The genesis of the present invention lay in the realization that known iontophoretic drug delivery processes have an efficiency in the range of about 5% or less and that iontophoretic drug delivery is largely a diffusion dependent process. This means that approximately 95% of the current utilized in known iontophoresis processes is consumed in activities other than delivering the intended drug. For example, much current is wasted by the migration of highly mobile species such as H+, OH-, Na and Cl-.
- Thus it was realized that iontophoretic drug delivery efficiency would be enhanced if the availability of species which are more mobile than the drug which was to be delivered were minimized. Minimization of the concentration or charge of species which were more easily transported than the intended species (i.e. a drug) is utilized herein to provide enhanced drug delivery. The enhanced drug delivery described herein may permit iontophoresis to become a viable alternative to other drug delivery techniques.
- Prior art iontophoretic devices often utilize substantially inert stainless steel, nickel or other nickel and iron alloys as current distribution members or electrodes. During operation of such iontophoretic devices in accordance with prior art iontophoretic drug delivery methods, electrolysis of water occurs. Hydronium (H+) ions are formed at the anode and hydroxide ions (OH-) are produced at the cathode. In addition, gaseous hydrogen and oxygen are evolved at the cathode and anode, respectively. (Use of nickel or nickel-containing alloys, e.g. stainless steel, also occasionally results in the formation of nickel ions at the anode. The nickel ions are then free to migrate into the drug reservoir of the device and from there into the body.)
- Iontophoretic devices which employ such essentially inert electrodes have several inherent disadvantages. First, they exhibit reduced coulombic efficiency of drug transfer (i.e. of charged species) due to the formation of highly mobile hydronium and hydroxide ions at the electrodes. In addition, such devices may evidence instability of pH in the anodic and cathodic reservoirs and adjacent the skin due to the formation of hydronium or hydroxide ions and gaseous products (hydrogen and oxygen) at the electrodes. Lastly, as noted above, while prior art iontophoretic electrodes are substantially electrochemically inert, some undesirable oxidation, e.g. of nickel or other alloy metals, does occur.
- These disadvantages mean that known iontophoretic devices used according to conventional drug delivery methods have the following drawbacks:
- 1) Lower coulombic efficiency requires that the battery for a portable or ambulatory device be larger (i.e. of higher capacity). In addition, the voltage required to maintain a certain therapeutic dose rate becomes larger as the coulmbic efficiency becomes smaller.
- 2) The shift in pH in the cathodic and/or anodic reservoirs, which may for example be in gel form, that is caused by the electrolysis of water may cause skin irritation, possible degradation of the physical properties of the gel components of the apparatus or may change the activity of the drug.
- 3) The formation of hydrogen and oxygen gas at the electrodes can result in a loss of contact between the electrodes and any cathodic or anodic reservoirs leading to reduced apparatus performance.
- 4) The oxidation of nickel or other metals at the anode may result in the contamination of the anodic reservoir with metal ions which then are free to migrate into the skin and body with possible deleterious effects.
- It is to overcome these disadvantages and increase the overall efficiency of the iontophoresis process that the present invention was made.
- One method contemplated by the present invention for reducing the formation of undesirable or undesired hydronium ions at an electrode and to reduce contamination of the drug reservoir due to the oxidation of electrode metal is to select intentionally an electrode (e.g. an anode) comprising an electrochemically active or sacrificial component which, when oxidized or reduced during operation of the device, produces a species which immediately reacts with ions (e.g. anions) present in the electrode assembly or available to the electrode, e.g. in the drug reservoir (which also may be specifically selected), to form an insoluble salt or neutral chemical compound, e.g. H20. "Sacrificial" as that term is used herein means that at least a portion of the electrode (whether anode or cathode) is electrochemically oxidized or reduced during transdermal drug delivery. "Electrochemically active", as the term is used herein, means "sacrificial" as defined above, but includes a material that is not itself oxidized or reduced but which participates in oxidation / reduction. The anion or cation present in the drug reservoir can be present as a separately added material or as the counter-ion to an ionic or cationic drug species to be delivered. Illustrating this practice of the invention, the chloride (or hydrochloride) form of a positively charged drug (D+) could be chosen to be delivered (e.g. by adding it to the reservoir) and the anode could have a silver electrochemically active component which would be sacrificed by oxidation during iontophoresis. Thus, it is seen that the design of the sacrificial of the electrochemically active component of the electrode / drug reservoir system can require the selection of a appropriate electrode material, or electrode construction and/or drug or drug salt.
- By this expedient, i.e. precipitation of an insoluble species, silver ions and chloride ions are removed from the drug delivery systems and thus are not available to consume electrical charge from the device. The efficiency of delivery of the desired species (i.e. the coulomic efficiency) is increased because unwanted species such as Ag+ and Cl- are simply removed from the system. Furthermore, production of H+ is minimized or avoided thus minimizing pH variation and 02 production.
- In an analogous fashion, if a neutral species (rather than one which precipitates from the system) is formed from undesired ions there is again a net removal of unwanted species since neutral species also would not reduce the efficiency of delivery of charged drug species by migrating in response to an electrical potential gradient.
- Possible electrode electrochemically active component materials and drug anions for sacrificial electrode devices are numerous, but in general, silver, copper and molybdenum metals form insoluble halide salts (e.g. AgCl, AgI, AgBr, CuCl, CuI, CuBr, MoCl3, MoI2) and therefore are possible sacrificial anode candidates for delivery of cationic drugs. In addition, ferro and ferricyanides of many metals (e.g. Ag, Sn, Zn, Ni, Mn) are insoluble and therefore combination of these metals with ion cyanide doped reservoirs may provide suitable sacrificial anode/drug reservoir systems.
- The silver anode/drug chloride sacrificial system is particularly preferred for two reasons. First, silver chloride is highly insoluble and second, many cationic drugs can be purchased in the hydrochloride form which means that the chloride anion in the drug reservoir will be present as the counterion to the drug cation. During operation of an iontophoretic device with a silver anode (e.g. a silver current distribution member) and a chloride-containing reservoir, silver is oxidized (Ag → Ag + e ) and then reacts with the chloride ion to form insoluble silver chloride near the surface of the silver anode (Ag + Cl- → AgCl). Simultaneously, the drug cation migrates from the reservoir into the body with greater efficiency than if the oxidation of water to form hydronium ion were allowed to occur at the anode if the anode were substantially inert, i.e. if it had no electochemi- cally active component.
- An example of a system where the anion in the drug reservoir is present as an additive is the copper /potassium ferrocyanide system. When K3Fe(CN)6 is added to the drug reservoir, Fe(CN)6 3- anions are formed. By placing the drug reservoirs in contact with,e.g. a copper anode, the insoluble salt Cu3Fe(CN)6 will be formed during device operation. However, unlike the silver/chloride system where the drug cation migrates into the body, in this system the potassium ions will be free to migrate from the drug reservoir into the body.
- Generally speaking, then a further practice of this aspect of the invention would be to employ DXFe(CN)6 (x is an integer greater than 0) rather than K3Fe(CN)61 where it is desired to transport a drug (D+) species through the skin without cationic, e.g. K+, competition.
- In an analogous practice of this invention, negatively charged, anionic drug species may be more efficiently delivered if an electrochemically active component of the cathode is intentionally selected utilizing the precepts of this invention.
- An example of a sacrificial cathode electrochemically active material of this invention is chloridized silver. During device operation, the AgCl on the surface of a silver cathode is decomposed to give silver metal and chloride anion (AgCl+ e- → Ag + Cl-). The chloride anion is free to migrate, along with any anionic drug, into the body. In this respect, the Ag/AgCl sacrifical cathode is less efficient than the silver/chloride sacrificial in that chloride ion is produced and is delivered to the body. However, the beneficial aspects of the Ag/AgCl cathode include (a) no hydrogen gas formation and (b) no hydroxyl anions produced at the cathode.
- One skilled in this art will recognize that a sacrificial cathode of this generic type generally comprises a metallic salt in contact with a metal cathode. Furthermore, device operation must result in the decomposition fo the metallic salt to form a metal in reduced form plus an anion. If both these conditions are met, in this practice of the present invention anionic drugs are delivered with mitigation of pH changes.
- The use of a sacrificial cathode as herein described in conjunction with an anionic drug specifically selected so that the counter-ion will react with the anion being produced at the cathode to form an insoluble salt or neutral compound provides an equivalent method for the control of ion transport as outlined for the anode and anodic reservoir.
- Two examples of anionic drug (D ) which could be intentionally selected for use with an Ag/AgCl cathode (these drugs would likely to dispersed or dissolved in the ion drug reservoir) are silver or copper salicylate. In this system, chloride ions formed at the cathode are free to react with silver or copper ions in the drug reservoir to form an insoluble salt thus allowing the negatively charged D- anion to migrate in to the body without anionic competition.
- In yet another method contemplated by the present invention to minimize the formation of hydronium and hydroxide ions which consume current and reduce efficiencies, an intercalation-type cathode or anode is employed. Intercalation electrodes have the property of being capable of reducing alkali metal ions, e.g. sodium and potassium. The use of intercalation-type cathode or anode materials is particularly advantageous in that the formation of hydroxyl and hydronium ion is minimized along with a decline in the production of hydrogen or oxygen gas.
- It is to be recognized that electrodes comprising intercalation-type materials may be used either on the anode or the cathode of the iontophoresis device and thus can deliver either positively or negatively charged drugs. This can be illustrated for sodium tungstate where the anodic reaction would be:
-
- In yet another practice of the instant invention in which the overall coulombic efficiency of a given iontophoretic drug delivery device is enhanced, a metallic or amalgam electrode is employed optionally in conjunction with the addition of specific metal cations to the drug reservoir, e.g. optionally with selection of a drug having a specific metal cation. In this practice of the invention the amalgam electrode is consumed during electrochemical discharge of the apparatus, and it reacts with a species intentionally made available to the electo- chemical oxidation /reduction product of the amalgam, e.g. by adding a selected drug to the system such as in the drug reservoir. Thus, as described above, the amalgam material herein described is electrochemically reacted and undesired, highly mobile, charged species are consumed or removed. As with the intercalation-type cathode materials discussed above, the production of hydroxyl and hydronium ions during electrochemical discharge also is reduced. Again pH stability is obtained, thus increasing the overall stability and efficiency of the drug delivery device.
- A yet further method for preventing the formation of hydroxyl ions and hydrogen gas at the cathode is to select intentionally an anionic drug whose counter-ion is an easily reducible metal such as silver or copper (e.g. a metal ion reducible to the metal from aqueous solution). During operation of a device whose reservoir contains such a metal species, the metal ion is reduced to form the neutral metal and the drug anion is free to migrate and carry charge toward the anode. To generalize, any form of the anionic drug of interest having reducible metal ions may be selected. The metal ion of the drug is reduced to a neutral species, i.e. it is plated out or effectively immobilized, and the drug anion is free to migrate and carry charge toward the anode.
- To this point, the present invention has been described in terms of specific selection of drugs or electrode materials so that the formation of water electrolysis products (and the problems thereby created) are minimized. However, the present invention is not limited to electrode material/drug selections where the electrode component is electrochemically oxidized or reduced during operation of the iontophoresis device. The invention may be practised with presently available "inert" electrodes if it is realized that their efficiency may be significantly enhanced by the judicious, intentional selection of the drug to be delivered. Generally speaking, the use of inert electrodes to deliver drugs is accomplished by selecting either the basic (e.g. OH- or amine) or acid (H+) form of the drug to be delivered depending upon whether an anionic or cationic form of the drug is to be delivered. Weak acid or weak base forms constitute a preferred class of such drugs. For example, oxidation of water proceeds according to the half reaction, H2O → 2H+ + 1/2 02 + 2e . Thus if the basic form of the drug to be delivered (DOH) is selected the reaction H+ + DOH → H2O + D+ would occur, preferably in the drug reservoir. By this choice of drug form or drug precursor, hydronium ion is removed by conversion to the neutral species, water, and the concentration of D+ is increased. Conversely, the reduction of water occurs according to the half reaction, H20 + e → OH + 1/2H2. If it is desired to deliver the acid (hydronium) form of the drug, then the reaction OH + HD → H2O + D would occur, thereby removing hydroxyl ions and increasing D concentration. This application of the present invention suggests that if either a desired acid or basic form of a specific ionically delivered drug is not available, synthesis for purposes of enhanced iontophoretic drug delivery could be accomplished.
- Two observations should be made regarding the description of the present invention in the previous paragraph. First, as described, an inert electrode is employed to oxidize or reduce water. The electrochemically active component of the drug delivery apparatus (e.g. a stainless steel or platinum electrode component) participates in the iontophoretic drug delivery process without itself being electrochemically changed or consumed. Second, even though undesirable hydroxyl and hydronium ions are formed, by the including or selecting of a drug with the specified balancing or counter ion, deleterious pH changes are minimized and hydronium ions and hydroxyl ions are converted to neutral water. In this practice of the invention, the production of gaseous species, i.e. H2 and 02, occurs and thus the sacrificial methods earlier described should be chosen if gas evolution is to be avoided.
- Stated generally therefore, where the ionic drug species to be delivered iontophoretically is a cation then the counteranion is preferably either a metal ion which in the redox conditions of the electrode assembly can plate onto or be absorbed into the cathode or an anion which reacts with cations generated at the cathode to produce a neutral species (eg water, a solid precipitate, or a neutral complex), or an ionic species of relatively low susceptibility to iontophoretic delivery from the electrode assembly. On the other hand, where the drug species is an anion then its counterca- tion is preferably such as to react with anions generated at the anode to produce a neutral species or an ionic species of relatively low susceptibility to iontophoretic delivery from the electrode assembly.
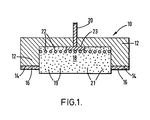
- A preferred emboidment of the present invention will now be described by way of exmaple and with reference to the accompanying drawing, Figure 1, which is a cross sectional view of one embodiment of the electrode assembly of the apparatus of the invention.
- In Figure 1 there is depicted, schematically, in cross section, a single substantially disc-
like electrode assembly 10 which is intended for use in an iontophoretic drug delivery apparatus. It is to be understood thatelectrode assembly 10 is but one of the two electrodes necessary for successful operation of an iontophoresis device and that the source of electrical energy that may also be required is also not depicted in Figure 1. - Again referring to the figure,
electrode assembly 10 comprises a support orhousing 12 which is generally "U" shaped in cross section and which is preferably flexible. Thesupport 12 is preferably a flexible backing member, conveniently substantially flat in form. In a preferred embodiment,support 12 is produced from self-supporting polymeric foam. In this practice of the invention,perimeter surface 14 ofhousing 12 would optionally have disposed thereon a skin-compatible, pressure-sensitive,biomedical adhesive 16 which is intended to hold the electrode in place on the patient's skin during iontophoretic drug delivery. The iontophoresis device may be held in place by other means, e.g a strap, in which instance adhesive 16 would not be needed. Thus is it to be understood, as depicted,electrode assembly 10 contemplates drug delivery generally in the direction which appears as downwards in the Figure. - With further reference to the figure, there is shown a
drug reservoir 18, which in the illustrated embodiment of the invention is a gel orgel matrix 21 containing theionic drug species 19 which is to be transdermally introduced across the skin barrier. In a preferred practice of the invention, the self-supporting, skin-compatible gel matrix 21 for the drug would containsufficient drug 19 so that approximately a one molar solution (applying the definition of a molarity from solvent-solute interactions) would result. Drug concentrations (in the reservoir) in the range of 0.02M to l.OM or more can conveniently be employed in the practice of this invention. In a preferred practice, the lower reservoir drug concentration ranges (e.g. less than about 0.5 molar) can be used in the efficient devices described herein. It should be noted that any of a number of possible gel matrices may be employed, those being described in the previously mentioned Webster patent comprising a particularly preferred practice of this invention. Agar or polyvinylpyrrolidone gels also are advantageously employed herein. - Also in the figure, there is depicted an
exterior connector 20 which in this embodiment is a wire.Exterior connector 20 is in further electrical contact with a current distribution member comprising a tab orplate 23 in electrical contact with anoptional screen 22. In this embodiment, the current distribution member would comprise silver. (The current distribution member need not be pure silver. An exterior layer of silver is all that is needed.) The silver screen is optionally included only to increase the surface area of the current distribution member. - Thus, in operation, an external source of electrical energy (not shown) may be connected to
exterior connector 20 which is, in turn, electrically connected to the silvercurrent distribution member - It should be noted with reference to the cathodic description of the sacrificial electrode described above that the silver current distribution member shown could be a silver/silver chloride cathode.
Electrode assembly 10, as depicted, would be placed in contact with a patient's skin and pressed with sufficient firmness so that pressuresensitive adhesive 16 would hold thedrug reservoir 18 in contact therewith by means offlexible housing 12.Silver tab 20 would be electrically connected to a source of electrical energy, preferably a small battery. Utilization of a battery permits iontophoretic drug delivery without substantial interference with the normal activities of the patient. - It is within the contemplation of the present invention that stationary electrical supply sources be employed in which case it would likely be necessary for the patient to be substantially immobilised. Although not depicted, a second indifferent or cooperating electrode would then be placed in contact with the patient's skin at a site separate from but electrically adjacent to the site on which
electrode assembly 10 has been placed. Upon connection to a source of electrical energy, migration of charged species fromreservoir 18 would occur. In this embodiment of the invention, if for example the reservoir is assumed to contain therein propranolol hydrochloride or lithium chloride, thesilver tab 23 andsilver screen 22 anode would be electrochemically consumed to produce silver ions as above described. These silver ions would react immediately with the chloride ions also present to produce a neutral, substantially insoluble species. In this manner, enhanced delivery of propranolol or lithium would occur due to the fact that little electrolysis occurs. The silver chloride precipitation reaction removes silver and chloride ions from the reservoir, thus further enhancing efficiency. - Heretofore, the discussion has focussed upon the use of iontophoresis to treat humans. Obviously, the invention herein disclosed could be used with animals and should not be limited to humans.
- The present invention will now be illustrated by the following examples which should not be employed so as to limit the scope of this invention:
- In-vivo studies of iontophoretic drug delivery were run on New Zealand white rabbits. As indicated, the rabbits were in some studies sedated as with pentobarbital, and others were merely constrained. The sedation studies generally were conducted for a time period not exceeding 7 hours whereas the "constrained" studies were run for time periods of up to 30 hours. Each rabbit was used in a particular study only once.
- As is more completely described below, an iontophoretic device employing an electrode assembly as shown and described in Fig. 1 was used to introduce lithium (chloride), (sodium) salicylate or propranolol (hydrochloride) into the rabbits. The gel "reservoir" contained approximately a 1 molar concentration of each of the respective drugs. The device employed a silver anode and a silver/silver chloride cathode as described above.
- The iontophoretic device was placed posteriorly on the rabbit, the hair having been clipped and removed with a depilatory. The device was then attached by means of an adhesive for the duration of the experiment. During the experimental procedure, blood samples were removed from the subject rabbits. Where rabbits were anaesthetized, blood samples were removed from their inferior vena cava by means of a catheter inserted into the femoral vein. For the experiments employing constrained (rather than anaesthetized rabbits, blood samples were pulled from the heart by means of a catheter inserted into the marginal vein of the rabbit's ear. The samples thus withdrawn then were analyzed for the drug which was iontophoretically introduced therein.
- Employing the experimental procedure described in Example I, the drugs of interest were iontophoretically introduced into rabbits. Blood samples were withdrawn as described and analyzed, the concentration of the respective drugs being plotted as a function of time. The data so obtained then was fit to the expression
C = B(1-exP(-kit))
where "C" is the concentration of drug in the rabbit's blood at a particular time; "B" is the plateau drug concentration, i.e. the highest or "steady state" concentration achieved when drug input and drug consumption are in equilibrium; Ki is the iontophoretic decay constant; and "t" is time. Tables 1, 2 and 3 indicate values of these parameters for a number of runs (each "run" corresponding to numbers obtained from a given rabbit, indicated by letter, on a given day, indicated by number). The drugs delivered in Tables 1, 2 and 3 were lithium ion, salicylate ion and protonated propranolol ion, respectively. -
- For some of the rabbits tested, a known amount of a given drug was administered intravenously and the consumption of the drug by the animal was monitored as a function of time. From these data, values for the drug elimination decay constant (Ke) and the initial drug concentration (Co) were determined by plotting the natural logarithm of concentration (In C) versus time. Once the value of C0 and the intravenous dosage had been determined, the volume of distribution (Vd) was calculated using the expression
-
- The parameters listed in Tables 1, 2 and 3 can be used to estimate the efficiency of drug delivery. An estimate of the steady-state drug delivery rate (Rd) can be made by multiplying the plateau drug concentration (B) by the volume of distribution (Vd) and the drug elimination decay constant (ke), that is,
-
where M is the molecular weight of the drug ion, I is the current in milliamps and F is Faraday's constant. The efficiency of drug delivery (Er) can be estimated from the ratio Rd/Rt according to the expression -
- It is to be noted that for some of the runs, the value of Er exceeded 100%. This is possible since Rd includes a contribution due to passive diffusion of the drug through the skin, therefore the ration Rd/Rt can exceed unity.
- Also listed in Tables 1, 2 and 3 is the true coulombic efficiency (E ) for each experiment which was calculated by subtracting the passive drug delivery rate (Rp) from the total drug delivery rate (Rd), that is,
-
- It was found that total in-vivo drug delivery data, as defined in equation (1) of Example IV, was the sum of two contributions, one passive and the other iontophoretic. Thus, it was found that the rate of drug delivery (Rd) could be expressed as
where Rp is the rate of passive drug delivery and Ri is the rate of iontophoretic drug delivery. The rate of passive delivery depends on the area of contact and the drug concentration of the drug reservoir. The rate of iontophoretic delivery is directly proportional to the current used in the experiment, that is,
where E is the coulombic efficiency, I is the current and A is a proportionality constant whose value is dependent upon the molecular weight of the drug. - Substitution of the above expression for Ri into Equation (4) yields
-
- From the data obtained as described above, a plot of Rd versus current for lithium chloride, sodium salicylate and propranolol hydrochloride was made and a best linear fit obtained. The rates of passive drug delivery for each of these drugs then is determined by the intercept of this "fit". Values of this intercept are listed in Table 4. Also listed in Table 4 is the equivalent current for each drug. The equivalent current for a given drug is the current at which half of the drug delivery would occur via passive diffusion and half would occur iontophoretically.
- The slopes of the best linear fit of Rd versus current described above were used to estimate the coulombic efficiency (Ec) for in-vivo drug delivery. Table 5 compares the coulombic efficiency estimated from the in-vivo experiments to those determined from in-vitro drug delivery through excised rabbit skin and through polyvinyl alcohol (PVA) membrane into a 0.lM sodium chloride solution. The in-vitro drug delivery measurements were taken using a Franz diffusion cell commercially available from the Crown Glass Company, Somerville, N.J. U.S.A.
- The efficiency of in-vitro drug delivery through a PVA membrane is an indication of the relative mobilities of lithium and propranolol with respect to chloride ion, and salicylate with respect to sodium ion. The coulombic efficiency of drug transport through a PVA membrane probably represents an upper limit for the coulombic efficiency for the gels, electrodes and drug concentrations likely to be used in the in-vivo experiments.
- The data presented in Table 4 indicate that lithium and propranolol were transported approximately equally efficiently through excised and viable rabbit skin. Further the data indicate that salicylate was more effectively delivered through viable tissue than through excised skin
-
- To summarise, while there does appear to be a fair amount of scatter in the in-vivo data, we have found that the methods described herein provide a fairly reproducible method for determining coulombic efficiencies and passive drug delivery rates for in-vivo studies. The efficiencies so calculated appear to be in substantial agreement with similar efficiencies computed from in-vitro experiments.
- A number of anode/cathode drug combinations and drug concentrations were evaluated with respect to their minimization of the production of undesired species. In particular, drug reservoir pH changes were measured, from which hydronium ion delivery rates were computed. (The drug passed through a PVA membrane and was delivered onto 0.06 M Na Cl). Further, using the mathematical treatment described above, drug delivery efficiencies were determined. Experimental conditions and efficiencies were measured for delivery of lithium ion, potassium ion and salicylate ion as indicated in Tables 6, 7, 8 and 9.
- A number of observations may be made about the systems tested. Systems numbered 1-6 of Table 6 are basically prior art systems.
- Undesirable water electrolysis products are produced and thus pH is shown to change fairly substantially as in "pH" column for systems 1, 2 and 3 in Table 7, 1 and 2 of Table 8 and 1 of Table 9.
- As evidenced in Tables 7, 8 and 9, hydronium delivery rates were generally higher, and drug delivery efficiencies were generally lower for prior art systems versus systems employing the present invention. For example, systems numbered 1, 2 and 3 in Table 7 may be compared with systems numbered 4-9 in Table 7. Similarly systems 1 and 2 in Table 8 should be compared with 3-6 in Table 8 and system 1 in Table 9 with 2-8 in Table 9.
- To summarize, in conjunction with the teaching above, a broadly-based, flexible approach to solving the problem of inefficiency/instability in iontophoretic drug delivery is disclosed. While this disclosure has focused specifically upon two cationic and one anionic drug, it will be appreciated that this invention is broadly applicable to the iontophoresis art. The attached claims should be so broadly construed.
-
Claims (15)
Applications Claiming Priority (4)
| Application Number | Priority Date | Filing Date | Title |
|---|---|---|---|
| US06/665,699 US4747819A (en) | 1984-10-29 | 1984-10-29 | Iontophoretic drug delivery |
| US06/665,698 US4744787A (en) | 1984-10-29 | 1984-10-29 | Iontophoresis apparatus and methods of producing same |
| US665698 | 1984-10-29 | ||
| US665699 | 1984-10-29 |
Publications (4)
| Publication Number | Publication Date |
|---|---|
| EP0182520A2 true EP0182520A2 (en) | 1986-05-28 |
| EP0182520A3 EP0182520A3 (en) | 1987-09-02 |
| EP0182520B1 EP0182520B1 (en) | 1992-03-25 |
| EP0182520B2 EP0182520B2 (en) | 2002-08-28 |
Family
ID=27099269
Family Applications (1)
| Application Number | Title | Priority Date | Filing Date |
|---|---|---|---|
| EP19850307771 Expired - Lifetime EP0182520B2 (en) | 1984-10-29 | 1985-10-28 | Apparatus for iontophoretic drug delivery |
Country Status (4)
| Country | Link |
|---|---|
| EP (1) | EP0182520B2 (en) |
| JP (1) | JP2584438B2 (en) |
| CA (1) | CA1267937A (en) |
| DE (1) | DE3585722D1 (en) |
Cited By (12)
| Publication number | Priority date | Publication date | Assignee | Title |
|---|---|---|---|---|
| WO1987004936A1 (en) * | 1986-02-12 | 1987-08-27 | Key Pharmaceuticals, Inc. | Method and apparatus for iontophoretic drug-delivery |
| EP0299631A2 (en) * | 1987-06-19 | 1989-01-18 | University of Utah Research Foundation | Flow-through methods and apparatus for iontophoresis application of medicaments at a controlled pH |
| EP0318776A1 (en) * | 1987-12-04 | 1989-06-07 | Robert Tapper | Method and apparatus for minimizing skin injury with electrode use |
| WO1991015260A1 (en) * | 1990-03-30 | 1991-10-17 | Alza Corporation | Device and method for iontophoretic drug delivery |
| US5084008A (en) * | 1989-12-22 | 1992-01-28 | Medtronic, Inc. | Iontophoresis electrode |
| US5135477A (en) * | 1984-10-29 | 1992-08-04 | Medtronic, Inc. | Iontophoretic drug delivery |
| EP0556112A1 (en) * | 1992-02-14 | 1993-08-18 | Elf Aquitaine | Iontophoresis device for transdermal delivery of a given total amount of an active agent to a subject |
| AU657681B2 (en) * | 1990-03-30 | 1995-03-23 | Alza Corporation | Device and method for iontophoretic drug delivery |
| WO1995027530A1 (en) * | 1994-04-08 | 1995-10-19 | Alza Corporation | Electrotransport system with ion exchange competitive ion capture |
| WO1996017649A1 (en) * | 1994-12-05 | 1996-06-13 | Kabushiki Kaisya Advance | High efficiency electrode system for iontophoresis |
| WO1997011744A1 (en) * | 1995-09-29 | 1997-04-03 | Becton Dickinson And Company | Low-cost electrodes for an iontophoretic device |
| WO2007027892A1 (en) * | 2005-08-31 | 2007-03-08 | Alza Corporation | Cathode for electrotransport delivery of anionic drug |
Families Citing this family (3)
| Publication number | Priority date | Publication date | Assignee | Title |
|---|---|---|---|---|
| JPS62268570A (en) * | 1986-05-19 | 1987-11-21 | 株式会社アドバンス | Electrode for iontophoresis |
| JP3459724B2 (en) | 1996-03-17 | 2003-10-27 | 久光製薬株式会社 | Electrode device for iontophoresis |
| EP3308777A1 (en) * | 2008-06-19 | 2018-04-18 | LTS Lohmann Therapie-Systeme AG | Composition for transdermal delivery of cationic active agents |
Citations (2)
| Publication number | Priority date | Publication date | Assignee | Title |
|---|---|---|---|---|
| EP0058920A1 (en) * | 1981-02-23 | 1982-09-01 | Motion Control, Inc. | Bioelectrode |
| EP0097436A1 (en) * | 1982-06-16 | 1984-01-04 | Minnesota Mining And Manufacturing Company | Bioelectrode |
Family Cites Families (2)
| Publication number | Priority date | Publication date | Assignee | Title |
|---|---|---|---|---|
| US3964477A (en) * | 1975-01-30 | 1976-06-22 | Sybron Corporation | Method of using electrodes having antiseptic properties for LIDC therapy |
| JPS5810066A (en) * | 1981-07-10 | 1983-01-20 | 株式会社アドバンス | Plaster structure for ion tofuorese |
-
1985
- 1985-10-24 CA CA000493757A patent/CA1267937A/en not_active Expired - Lifetime
- 1985-10-28 JP JP60241249A patent/JP2584438B2/en not_active Expired - Lifetime
- 1985-10-28 DE DE8585307771T patent/DE3585722D1/en not_active Expired - Lifetime
- 1985-10-28 EP EP19850307771 patent/EP0182520B2/en not_active Expired - Lifetime
Patent Citations (2)
| Publication number | Priority date | Publication date | Assignee | Title |
|---|---|---|---|---|
| EP0058920A1 (en) * | 1981-02-23 | 1982-09-01 | Motion Control, Inc. | Bioelectrode |
| EP0097436A1 (en) * | 1982-06-16 | 1984-01-04 | Minnesota Mining And Manufacturing Company | Bioelectrode |
Cited By (20)
| Publication number | Priority date | Publication date | Assignee | Title |
|---|---|---|---|---|
| US5135477A (en) * | 1984-10-29 | 1992-08-04 | Medtronic, Inc. | Iontophoretic drug delivery |
| WO1987004936A1 (en) * | 1986-02-12 | 1987-08-27 | Key Pharmaceuticals, Inc. | Method and apparatus for iontophoretic drug-delivery |
| US4886489A (en) * | 1986-03-19 | 1989-12-12 | Jacobsen Stephen C | Flow-through methods and apparatus for iontophoresis application of medicaments at a controlled pH |
| EP0299631A2 (en) * | 1987-06-19 | 1989-01-18 | University of Utah Research Foundation | Flow-through methods and apparatus for iontophoresis application of medicaments at a controlled pH |
| EP0299631A3 (en) * | 1987-06-19 | 1990-04-11 | University of Utah Research Foundation | Flow-through methods and apparatus for iontophoresis application of medicaments at a controlled ph |
| EP0318776A1 (en) * | 1987-12-04 | 1989-06-07 | Robert Tapper | Method and apparatus for minimizing skin injury with electrode use |
| US5084008A (en) * | 1989-12-22 | 1992-01-28 | Medtronic, Inc. | Iontophoresis electrode |
| AU657681B2 (en) * | 1990-03-30 | 1995-03-23 | Alza Corporation | Device and method for iontophoretic drug delivery |
| WO1991015260A1 (en) * | 1990-03-30 | 1991-10-17 | Alza Corporation | Device and method for iontophoretic drug delivery |
| US5423739A (en) * | 1990-03-30 | 1995-06-13 | Alza Corporation | Device and method for iontophoretic drug delivery |
| US5558633A (en) * | 1990-03-30 | 1996-09-24 | Medtronic, Inc. | Device and method for iontophoretic drug delivery |
| EP0556112A1 (en) * | 1992-02-14 | 1993-08-18 | Elf Aquitaine | Iontophoresis device for transdermal delivery of a given total amount of an active agent to a subject |
| FR2687321A1 (en) * | 1992-02-14 | 1993-08-20 | Elf Aquitaine | IONOPHORESIS DEVICE FOR THE TRANSCUTANEOUS ADMINISTRATION OF A TOTAL QUANTITY GIVEN FROM AN ACTIVE PRINCIPLE TO A SUBJECT. |
| WO1995027530A1 (en) * | 1994-04-08 | 1995-10-19 | Alza Corporation | Electrotransport system with ion exchange competitive ion capture |
| US6049733A (en) * | 1994-04-08 | 2000-04-11 | Alza Corporation | Electrotransport system with ion exchange material competitive ion capture |
| WO1996017649A1 (en) * | 1994-12-05 | 1996-06-13 | Kabushiki Kaisya Advance | High efficiency electrode system for iontophoresis |
| US5766144A (en) * | 1994-12-05 | 1998-06-16 | Kabushiki Kaisya Advance | High efficiency electrode system for iontophoresis |
| WO1997011744A1 (en) * | 1995-09-29 | 1997-04-03 | Becton Dickinson And Company | Low-cost electrodes for an iontophoretic device |
| US6584349B1 (en) | 1995-09-29 | 2003-06-24 | Vyteris, Inc. | Low cost electrodes for an iontophoretic device |
| WO2007027892A1 (en) * | 2005-08-31 | 2007-03-08 | Alza Corporation | Cathode for electrotransport delivery of anionic drug |
Also Published As
| Publication number | Publication date |
|---|---|
| EP0182520B2 (en) | 2002-08-28 |
| EP0182520B1 (en) | 1992-03-25 |
| CA1267937A (en) | 1990-04-17 |
| EP0182520A3 (en) | 1987-09-02 |
| JP2584438B2 (en) | 1997-02-26 |
| DE3585722D1 (en) | 1992-04-30 |
| JPS61149168A (en) | 1986-07-07 |
Similar Documents
| Publication | Publication Date | Title |
|---|---|---|
| US4744787A (en) | Iontophoresis apparatus and methods of producing same | |
| US4747819A (en) | Iontophoretic drug delivery | |
| US5135477A (en) | Iontophoretic drug delivery | |
| EP0182520B1 (en) | Apparatus for iontophoretic drug delivery | |
| US5084008A (en) | Iontophoresis electrode | |
| EP0400118B1 (en) | Iontophoresis electrode | |
| EP1115454B1 (en) | Controlled dosage drug delivery system | |
| US7398121B2 (en) | Iontophoresis device | |
| US5057072A (en) | Iontophoresis electrode | |
| JP3462522B2 (en) | Iontophoresis device for transdermal administration of a given total amount of active ingredient to a patient | |
| JPWO2007026672A1 (en) | Versatile electrolyte composition for iontophoresis | |
| EP0429552B1 (en) | Iontophoresis electrode | |
| US5807305A (en) | Iontophoresis device comprising at least one electrode assembly with a reversible composite electrode | |
| Phipps et al. | IONTOPHORETIC DRUG DELIVERY: ADVANTAGES AND LIMITATIONS |
Legal Events
| Date | Code | Title | Description |
|---|---|---|---|
| PUAI | Public reference made under article 153(3) epc to a published international application that has entered the european phase |
Free format text: ORIGINAL CODE: 0009012 |
|
| AK | Designated contracting states |
Kind code of ref document: A2 Designated state(s): DE FR GB NL |
|
| PUAL | Search report despatched |
Free format text: ORIGINAL CODE: 0009013 |
|
| AK | Designated contracting states |
Kind code of ref document: A3 Designated state(s): DE FR GB NL |
|
| 17P | Request for examination filed |
Effective date: 19880224 |
|
| 17Q | First examination report despatched |
Effective date: 19901120 |
|
| GRAA | (expected) grant |
Free format text: ORIGINAL CODE: 0009210 |
|
| AK | Designated contracting states |
Kind code of ref document: B1 Designated state(s): DE FR GB NL |
|
| REF | Corresponds to: |
Ref document number: 3585722 Country of ref document: DE Date of ref document: 19920430 |
|
| ET | Fr: translation filed | ||
| PLBI | Opposition filed |
Free format text: ORIGINAL CODE: 0009260 |
|
| 26 | Opposition filed |
Opponent name: ALZA CORPORATION Effective date: 19921221 Opponent name: SOCIETE NATIONALE ELF AQUITAINE Effective date: 19921218 Opponent name: BECTON, DICKINSON AND COMPANY Effective date: 19921214 |
|
| NLR1 | Nl: opposition has been filed with the epo |
Opponent name: ALZA CORPORATION Opponent name: SOCIETE NATIONALE ELF AQUITAINE Opponent name: BECTON, DICKINSON AND COMPANY. |
|
| REG | Reference to a national code |
Ref country code: GB Ref legal event code: 732E |
|
| RAP2 | Party data changed (patent owner data changed or rights of a patent transferred) |
Owner name: ALZA CORPORATION |
|
| NLS | Nl: assignments of ep-patents |
Owner name: ALZA CORPORATION TE PALO ALTO, CALIFORNIE, VER. ST |
|
| REG | Reference to a national code |
Ref country code: FR Ref legal event code: TP |
|
| PLBQ | Unpublished change to opponent data |
Free format text: ORIGINAL CODE: EPIDOS OPPO |
|
| PLAB | Opposition data, opponent's data or that of the opponent's representative modified |
Free format text: ORIGINAL CODE: 0009299OPPO |
|
| R26 | Opposition filed (corrected) |
Opponent name: BECTON, DICKINSON AND COMPANY * 921218 SOCIETE NAT Effective date: 19921214 |
|
| NLR1 | Nl: opposition has been filed with the epo |
Opponent name: ALZA CORPORATION Opponent name: SOCIETE NATIONALE ELF AQUITAINE Opponent name: BECTON, DICKINSON AND COMPANY |
|
| RDAH | Patent revoked |
Free format text: ORIGINAL CODE: EPIDOS REVO |
|
| APAC | Appeal dossier modified |
Free format text: ORIGINAL CODE: EPIDOS NOAPO |
|
| APAE | Appeal reference modified |
Free format text: ORIGINAL CODE: EPIDOS REFNO |
|
| APAC | Appeal dossier modified |
Free format text: ORIGINAL CODE: EPIDOS NOAPO |
|
| PLBQ | Unpublished change to opponent data |
Free format text: ORIGINAL CODE: EPIDOS OPPO |
|
| PLAB | Opposition data, opponent's data or that of the opponent's representative modified |
Free format text: ORIGINAL CODE: 0009299OPPO |
|
| PLAB | Opposition data, opponent's data or that of the opponent's representative modified |
Free format text: ORIGINAL CODE: 0009299OPPO |
|
| APAC | Appeal dossier modified |
Free format text: ORIGINAL CODE: EPIDOS NOAPO |
|
| R26 | Opposition filed (corrected) |
Opponent name: BECTON, DICKINSON AND COMPANY * 19921218 SOCIETE N Effective date: 19921214 |
|
| REG | Reference to a national code |
Ref country code: GB Ref legal event code: IF02 |
|
| PLAW | Interlocutory decision in opposition |
Free format text: ORIGINAL CODE: EPIDOS IDOP |
|
| R26 | Opposition filed (corrected) |
Opponent name: VYTERIS INC. * 19921218 SOCIETE NATIONALE ELF AQUI Effective date: 19921214 |
|
| NLR1 | Nl: opposition has been filed with the epo |
Opponent name: VYTERIS INC. Opponent name: ALZA CORPORATION Opponent name: SOCIETE NATIONALE ELF AQUITAINE Opponent name: BECTON, DICKINSON AND COMPANY |
|
| PUAH | Patent maintained in amended form |
Free format text: ORIGINAL CODE: 0009272 |
|
| STAA | Information on the status of an ep patent application or granted ep patent |
Free format text: STATUS: PATENT MAINTAINED AS AMENDED |
|
| 27A | Patent maintained in amended form |
Effective date: 20020828 |
|
| AK | Designated contracting states |
Kind code of ref document: B2 Designated state(s): DE FR GB NL |
|
| NLR2 | Nl: decision of opposition | ||
| NLR3 | Nl: receipt of modified translations in the netherlands language after an opposition procedure | ||
| ET3 | Fr: translation filed ** decision concerning opposition | ||
| PGFP | Annual fee paid to national office [announced via postgrant information from national office to epo] |
Ref country code: NL Payment date: 20041003 Year of fee payment: 20 |
|
| PGFP | Annual fee paid to national office [announced via postgrant information from national office to epo] |
Ref country code: FR Payment date: 20041008 Year of fee payment: 20 |
|
| PGFP | Annual fee paid to national office [announced via postgrant information from national office to epo] |
Ref country code: DE Payment date: 20041021 Year of fee payment: 20 |
|
| PGFP | Annual fee paid to national office [announced via postgrant information from national office to epo] |
Ref country code: GB Payment date: 20041027 Year of fee payment: 20 |
|
| APAH | Appeal reference modified |
Free format text: ORIGINAL CODE: EPIDOSCREFNO |
|
| PG25 | Lapsed in a contracting state [announced via postgrant information from national office to epo] |
Ref country code: GB Free format text: LAPSE BECAUSE OF EXPIRATION OF PROTECTION Effective date: 20051027 |
|
| PG25 | Lapsed in a contracting state [announced via postgrant information from national office to epo] |
Ref country code: NL Free format text: LAPSE BECAUSE OF EXPIRATION OF PROTECTION Effective date: 20051028 |
|
| REG | Reference to a national code |
Ref country code: GB Ref legal event code: PE20 |
|
| NLV7 | Nl: ceased due to reaching the maximum lifetime of a patent |
Effective date: 20051028 |